How Long Does Tooth Extraction Take to Heal? Dentist’s Tips for Faster Recovery
Tooth extraction is one of the most common dental procedures, yet many patients feel anxious about the recovery process. Understanding how long tooth extraction takes to heal can help you prepare mentally and physically for what lies ahead. The healing timeline varies significantly depending on whether you’re having a simple extraction or a more complex surgical removal, your overall health, and how well you follow post-operative care instructions.
Recovery from tooth extraction isn’t a single event—it’s a multi-stage process that unfolds over weeks and months. While the initial socket may close within 7-10 days, complete bone healing can take several months. In this comprehensive guide, we’ll walk you through each phase of extraction healing, backed by professional dental recommendations and practical tips to accelerate your recovery.
Understanding the Extraction Healing Timeline
The healing process after tooth extraction follows a predictable biological pattern, though individual variations exist. According to the American Dental Association (ADA), most extraction sites progress through distinct healing phases. Simple extractions typically heal faster than surgical extractions because they involve less trauma to surrounding bone and soft tissue.
Simple extractions—where the tooth is loosened and removed without surgical intervention—usually result in socket closure within 7-10 days. Surgical extractions, which involve bone removal or tooth sectioning, may take 2-3 weeks for initial closure. However, the bone beneath continues remodeling for 3-6 months after the procedure. This is why dentists often recommend waiting 3-4 months before placing dental implants—the bone needs time to stabilize and achieve sufficient density.
Temperature sensitivity, slight swelling, and minor discomfort are normal during the first week. These symptoms shouldn’t persist beyond 2-3 weeks; if they do, contact your dentist immediately. Understanding what’s normal versus concerning helps you manage expectations and identify potential problems early.
Immediate Post-Extraction Care (First 24 Hours)
The first day after extraction is critical for establishing proper healing conditions. Your dentist will place a gauze pad over the extraction socket and ask you to bite down firmly for 30-45 minutes. This pressure helps form a blood clot, which is essential for protecting the socket and initiating healing. The clot acts as a biological dressing and scaffold for new tissue formation.
During the first 24 hours, follow these essential guidelines:
- Keep biting pressure on gauze for the recommended time; change gauze every 30 minutes if bleeding continues
- Avoid rinsing, spitting, or touching the extraction site—these actions can dislodge the blood clot
- Apply ice packs for 20 minutes on, 20 minutes off during the first 6-8 hours to reduce swelling
- Keep your head elevated using extra pillows to minimize blood flow to the area
- Take prescribed pain medication before anesthesia wears off for better pain control
- Avoid smoking and alcohol for at least 72 hours—both impair healing and increase infection risk
- Don’t use straws for drinking; the suction can disturb the clot
Swelling typically peaks around 24-48 hours after extraction. This is normal and doesn’t indicate complications. Some patients experience jaw stiffness and difficulty opening their mouth fully; this usually resolves within 3-5 days as swelling decreases.
The First Week After Extraction
Days 2-7 represent the critical inflammatory phase of healing. Your body is actively fighting potential infection while forming new tissue. During this period, you may notice some blood-tinged saliva, which is normal. However, if you experience bright red bleeding that doesn’t stop after 30 minutes of pressure, contact your dentist.
Pain management during week one should gradually decrease. Most patients find over-the-counter pain relievers (ibuprofen or acetaminophen) sufficient, though your dentist may prescribe stronger medication if needed. Ibuprofen is often preferred because it reduces inflammation in addition to blocking pain. Take medication with food to avoid stomach irritation, and never exceed recommended dosages.
Starting on day 3-4, you can begin gentle warm salt water rinses (1/2 teaspoon salt in 8 ounces warm water) after meals and before bed. This promotes cleanliness without disturbing the clot. Avoid vigorous rinsing; let the solution gently flow over the area. Continue this routine for 7-10 days.
Your diet during the first week should consist of soft, cool foods. Smoothies (not through straws), yogurt, applesauce, mashed potatoes, and scrambled eggs are excellent choices. Avoid hot foods and beverages, which can increase bleeding and swelling. As healing progresses and comfort improves, gradually introduce room-temperature soft foods.
By the end of week one, you should notice significant improvement in swelling and pain. The extraction site may still feel tender, but acute symptoms should be diminishing. If pain or swelling is worsening at this point, it may indicate dry socket or infection—conditions requiring immediate dental attention.
Weeks 2-4: Secondary Healing Phase
During weeks 2-4, the socket begins filling with new bone and soft tissue. Swelling should be minimal by day 10-14, and you can resume most normal activities. However, avoid strenuous exercise, heavy lifting, and intense physical activity for at least 3-4 days after extraction, as increased blood pressure can cause bleeding and delay healing.
The extraction site may appear to have a white or yellowish surface during this phase. This isn’t infection—it’s granulation tissue, a normal part of healing. It will gradually be replaced by bone and gum tissue. If you notice red, swollen, or painful areas, or if discharge is present, contact your dentist.
By week 2, most patients can resume normal oral hygiene around the extraction site, being careful not to disturb healing tissue. Use a soft-bristled toothbrush and avoid the extraction area for at least 7-10 days. When you do begin cleaning around it, be extremely gentle.
Cold sensitivity in adjacent teeth is common during weeks 2-4. This typically resolves as the gums heal and recede slightly. If sensitivity persists beyond 4-6 weeks, mention it to your dentist—it may indicate a separate issue requiring treatment.
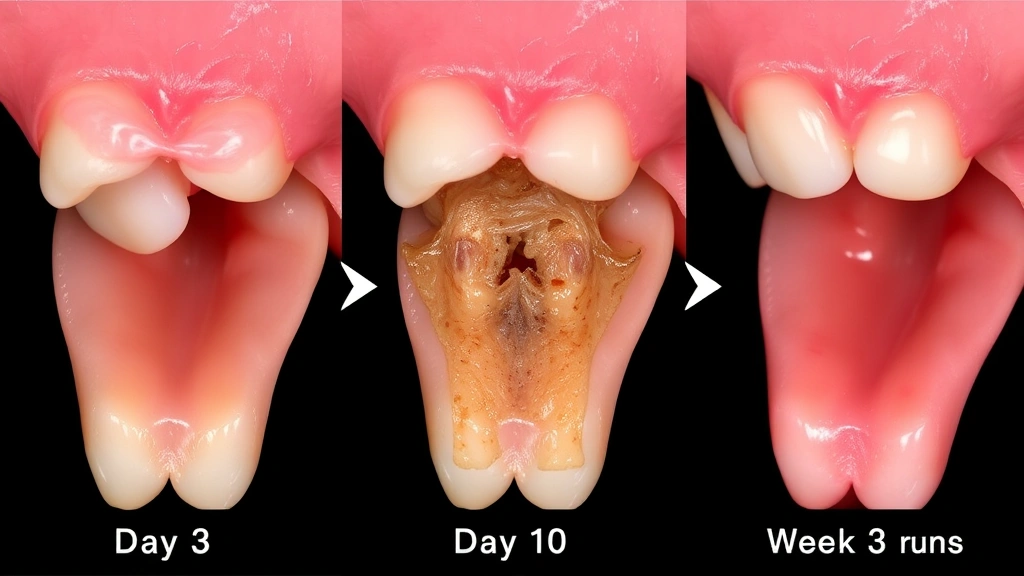
Long-Term Healing and Bone Integration
While the gum surface appears healed by week 3-4, significant biological changes continue beneath. Complete bone healing and remodeling takes 3-6 months, with some sources suggesting up to 12 months for full maturation. This is why building standards and medical guidelines emphasize patience in surgical recovery.
During months 2-3, bone loss becomes noticeable. The extraction socket naturally fills with bone, but the ridge often becomes narrower and shorter than the original tooth root. This bone resorption is normal but important to understand, especially if you’re planning future dental work like implants.
If you’re considering a dental implant, your dentist may recommend waiting 3-4 months to allow initial bone healing, or may suggest bone grafting if significant resorption occurs. Some patients need bone augmentation before implant placement. This decision should be made with your dentist based on extraction complexity and bone quality.
Temporary bridges or partial dentures can often be worn after 2-3 weeks, though they may need adjustment as bone resorbs. Avoid putting pressure on the extraction site during the first month.
Foods and Nutrition for Optimal Healing
Nutrition plays a crucial role in extraction healing. Your body requires specific nutrients to form new bone and soft tissue effectively. Protein is essential for tissue repair, while calcium and vitamin D support bone healing. Vitamin C promotes collagen formation, and zinc aids immune function.
Week 1 soft food suggestions:
- Protein: Greek yogurt, cottage cheese, soft scrambled eggs, protein shakes, bone broth
- Fruits and vegetables: Mashed sweet potato, avocado, banana, applesauce, cooked carrots
- Grains: Oatmeal, soft bread soaked in milk, rice pudding
- Dairy: Milk, cheese, pudding, custard (all excellent calcium sources)
Weeks 2-4 additions:
- Soft fish and shellfish (salmon is excellent for omega-3s and vitamin D)
- Ground meat in soft preparations like meatloaf or shepherd’s pie
- Soft pasta with nutrient-rich sauces
- Legumes (beans, lentils) as protein sources
- Cooked vegetables, gradually increasing firmness
Stay hydrated throughout recovery. Drink plenty of water, herbal tea, and nutrient-dense beverages. Avoid hot drinks for the first week, as heat can increase bleeding. Continue taking any multivitamins your dentist recommends, and discuss specific nutritional supplementation if you have dietary restrictions.
Foods to avoid during the entire first month include crunchy items, spicy foods, hot beverages, sticky foods, and anything requiring vigorous chewing. These can irritate the healing site or dislodge the clot.
Common Complications and When to Call Your Dentist
Most extractions heal without complications, but knowing warning signs helps you seek timely care. Dry socket (alveolar osteitis) is the most common complication, occurring in 2-5% of extractions. It happens when the blood clot dislodges prematurely, exposing bone. Symptoms include severe pain (often 3-4 days after extraction), foul taste, and visible bone in the socket.
Contact your dentist immediately if you experience:
- Severe pain that worsens after day 3-4
- Fever above 101°F (38.3°C)
- Excessive bleeding that won’t stop with pressure
- Swelling that worsens after day 3-4
- Difficulty breathing or swallowing
- Pus or discharge from the socket
- Numbness or tingling that doesn’t improve after a few days
- Visible bone fragments in the socket
Infection can develop if bacteria enter the extraction site. Signs include fever, increasing pain, swelling, and discharge. Infections require antibiotics and professional cleaning. Prevention is far easier than treatment, making post-operative care instructions critical.
Nerve damage occasionally occurs during extraction, particularly with lower molars. Temporary numbness or tingling usually resolves within weeks, but permanent nerve damage is rare. Report any unusual sensations to your dentist.
Preventing Infection and Promoting Faster Recovery
Infection prevention should be your primary focus during healing. Following your dentist’s post-operative instructions meticulously is the best protection. This includes maintaining the blood clot, avoiding contamination, and keeping the area clean without disturbing healing tissue.
Several evidence-based strategies accelerate healing:
Oral hygiene: After day 3, gentle salt water rinses maintain cleanliness. Starting day 7-10, carefully brush around the healing site with a soft brush. Avoid the socket itself until fully healed.
Smoking cessation: If you smoke, quitting—even temporarily—dramatically improves healing. Smoking reduces oxygen availability, impairs immune function, and significantly increases infection and dry socket risk. Avoid smoking for at least one week, ideally longer.
Alcohol avoidance: Alcohol interferes with medication effectiveness and impairs immune function. Avoid alcoholic beverages for at least 72 hours, and longer if taking prescription pain medication.
Stress management: Stress impairs immune function. Practice relaxation techniques, get adequate sleep, and avoid strenuous activity during the first week.
Prescribed medications: Take antibiotics exactly as prescribed, even if you feel better. Complete the full course to prevent resistant bacteria. Pain medication should be taken as needed, but don’t exceed recommended doses.
Follow-up appointments: Attend any scheduled follow-up visits. Your dentist will monitor healing, remove stitches if needed, and address any concerns early.
Applying a warm compress after 48 hours can increase blood flow and promote healing. Heat should be applied gently for 15-20 minutes several times daily after the initial swelling phase.
FAQ
How long does a tooth extraction take to heal completely?
Complete healing takes 3-6 months for bone integration, though the gum surface appears healed within 2-3 weeks. Simple extractions heal faster than surgical extractions. For more detailed recovery information, consult your dentist.
Can I exercise after tooth extraction?
Avoid strenuous exercise for 3-4 days after extraction. Increased heart rate and blood pressure can cause bleeding and delay healing. Light walking is acceptable after 24-48 hours if you feel comfortable.
When can I eat normally after extraction?
You can gradually return to normal foods as comfort improves, typically by week 3-4. Stick to soft foods for the first week, then gradually introduce firmer foods as healing progresses.
Is some bleeding normal after extraction?
Light bleeding and blood-tinged saliva are normal for 24-48 hours. Bright red bleeding that persists after 30 minutes of pressure warrants a call to your dentist.
What causes dry socket?
Dry socket occurs when the protective blood clot dislodges prematurely. Risk factors include smoking, vigorous rinsing, using straws, and certain medications. Proper aftercare prevents most cases.
How much swelling is normal?
Swelling typically peaks 24-48 hours after extraction, then gradually decreases. Some swelling lasting 7-10 days is normal. If swelling worsens after day 3-4, contact your dentist.
When can I have a dental implant placed?
Most dentists recommend waiting 3-4 months after extraction for bone healing before implant placement. Bone grafting may be necessary if significant resorption occurs. Your dentist will assess your specific situation.
Can I use a straw after extraction?
No. The suction from straws can dislodge the blood clot, causing dry socket. Use a cup or glass for drinking for at least one week.
What medications should I take after extraction?
Your dentist will recommend pain management options, typically over-the-counter ibuprofen or acetaminophen, or prescription medication for more complex extractions. Take antibiotics exactly as prescribed to prevent infection.
How do I know if I have an infection?
Signs of infection include fever above 101°F, increasing pain and swelling after day 3-4, pus discharge, and foul taste or odor. Contact your dentist immediately if you suspect infection.


