Tunneling Wound Healing: Expert Insights & Timeline
Tunneling wounds represent one of the most challenging complications in wound care, particularly in construction and occupational injury contexts. Unlike surface wounds that heal predictably, tunneling wounds develop hidden passages beneath intact skin, creating pathways where infection can flourish undetected. Understanding the healing timeline and proper management techniques is essential for anyone working in building trades or managing workplace injuries on job sites.
A tunneling wound typically takes 2 to 6 weeks to heal, though complex cases can extend 8-12 weeks or longer depending on depth, contamination, and individual healing factors. The extended timeline occurs because the wound must heal from the inside outward, requiring consistent moisture management and professional assessment. This comprehensive guide explores the science behind tunneling wounds, realistic healing expectations, and evidence-based treatment protocols that construction professionals should understand.
What Is a Tunneling Wound
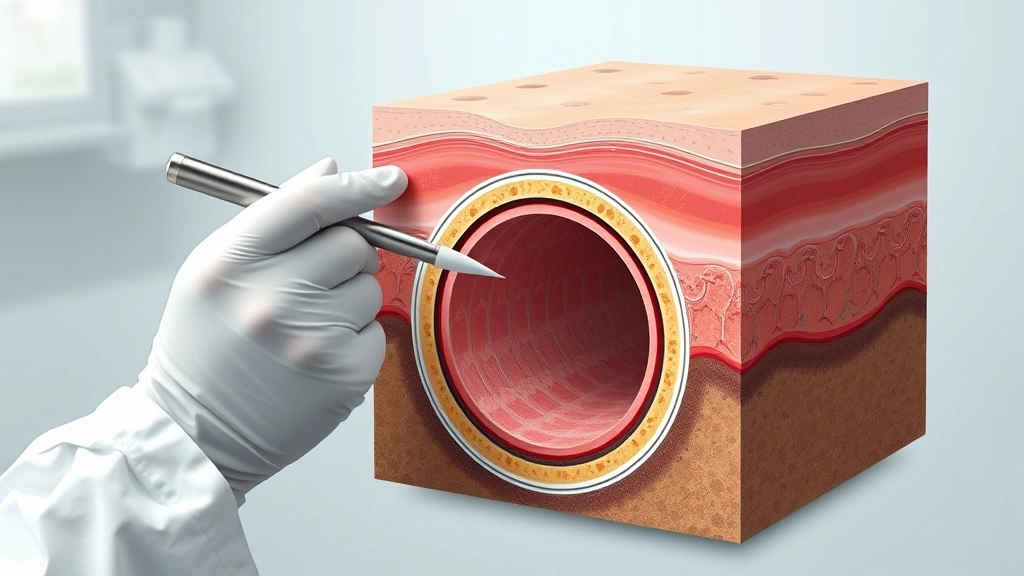
A tunneling wound, also called a sinus tract or undermined wound, occurs when tissue damage extends beneath the skin surface while the opening remains small and seemingly innocuous. Construction workers frequently encounter these injuries from puncture wounds, machinery accidents, or crush injuries that create deep channels under seemingly minor surface openings. The wound cavity extends horizontally or vertically beneath intact epidermis, creating a hidden space where bacteria thrive in anaerobic conditions.
The anatomical structure of tunneling wounds makes them particularly dangerous. The external opening may appear deceptively small—perhaps a quarter-inch diameter—while the actual tissue damage extends several inches beneath the surface. This discrepancy between visible damage and actual injury leads many people to underestimate severity and delay proper treatment. According to the Wound Care Society, approximately 15-20% of chronic wounds develop tunneling complications when inadequately managed initially.
Unlike pressure ulcers or diabetic foot wounds that develop gradually, traumatic tunneling wounds from construction accidents appear suddenly. The injury mechanism—whether from a nail puncture, machinery contact, or sharp object—determines the wound’s initial depth and contamination level. This makes proper on-site first aid and immediate professional evaluation critical for optimal outcomes.

Healing Timeline and Phases
Tunneling wound healing progresses through distinct phases, each with specific duration and characteristics. Understanding this timeline helps set realistic expectations and identify when complications may be developing.
Phase 1: Inflammatory Response (Days 1-5)
The first phase begins immediately after injury and involves the body’s natural inflammatory cascade. Blood clotting stops bleeding, while white blood cells migrate to the wound site to eliminate bacteria and remove debris. During this critical period, the wound opening may discharge blood-tinged fluid, and surrounding tissue appears red and swollen. Pain and localized warmth are normal responses as the immune system activates. For tunneling wounds, this phase determines whether infection establishes itself—proper cleaning and drainage are paramount during these first 24-48 hours.
Phase 2: Proliferative Stage (Days 5-21)
This phase represents the primary healing period for tunneling wounds, typically lasting 2-3 weeks. Fibroblasts produce collagen to rebuild tissue architecture, while new blood vessels form to restore circulation. The wound gradually fills from the base upward, with the tunnel progressively narrowing as new tissue develops. Proper moisture balance is critical during this phase; the wound needs enough moisture to support cell migration but not so much that maceration (softening) occurs. Regular dressing changes—typically every 2-3 days for tunneling wounds—allow healthcare providers to monitor cavity filling progress.
During this phase, the tunneling wound may produce moderate drainage containing serum and cellular material. This is normal and indicates active healing. However, foul-smelling discharge, excessive purulent material, or signs of spreading erythema suggest infection requiring immediate intervention.
Phase 3: Remodeling and Maturation (Weeks 3-12+)
The final healing phase involves tissue strengthening and scar maturation. Collagen reorganizes into stronger fiber patterns, and excess collagen is gradually removed. For straightforward tunneling wounds, this phase completes within 4-6 weeks total healing time. However, complex wounds with significant contamination or poor healing conditions may require 8-12 weeks or longer. During remodeling, the scar tissue gradually gains strength, eventually reaching approximately 80% of original tissue strength after several months.
The timeline varies considerably based on wound characteristics. A clean puncture wound in a young, healthy individual might heal in 3-4 weeks, while a contaminated tunneling injury in an immunocompromised person could require 3+ months. Construction workers returning to job sites should understand that even “healed” wounds remain vulnerable for weeks after closure, requiring protective measures to prevent reopening.
Factors Affecting Healing Duration
Multiple variables influence how quickly tunneling wounds heal, making individualized assessment essential for accurate timeline predictions.
Age and Overall Health Status
Younger individuals typically heal 20-30% faster than those over 65 due to enhanced cellular regeneration and stronger immune responses. Chronic conditions including diabetes, cardiovascular disease, and respiratory conditions significantly extend healing timelines. The CDC notes that diabetes alone increases healing time by 30-50% due to impaired white blood cell function and microvascular complications. Construction workers with pre-existing health conditions should inform healthcare providers immediately to establish realistic recovery expectations.
Infection Status
This represents the single most important factor determining healing duration. Uninfected tunneling wounds follow the standard 2-6 week timeline. However, infected wounds require antibiotics and often extended drainage management, extending healing to 8-12 weeks or longer. Biofilm formation—where bacteria organize into protective communities—particularly complicates recovery by resisting antibiotic penetration and immune system action. Recognizing early infection signs (increasing pain, foul odor, fever, spreading erythema) enables prompt intervention before biofilm establishment.
Wound Characteristics
The original injury mechanism significantly impacts healing duration. Puncture wounds with minimal surrounding tissue damage heal faster than crush injuries with extensive tissue trauma. Tunnel depth and length directly correlate with healing time; a 2-inch tunnel requires substantially longer healing than a half-inch tunnel. Contamination level also matters—clean wounds caused by sterile objects heal faster than dirty wounds from machinery or environmental exposure. When evaluating construction injuries, documenting the mechanism and contamination source helps predict probable healing timelines.
Nutritional Status and Hydration
Protein, vitamin C, and zinc are essential for collagen synthesis and immune function. Workers with inadequate nutrition—whether from poor diet or medical conditions affecting absorption—experience delayed healing. Proper hydration supports cellular processes and maintains skin turgor. Construction workers should maintain adequate nutrition during recovery, with particular attention to protein intake (1.2-1.5g per kilogram body weight) supporting wound healing.
Oxygenation and Circulation
Wounds require adequate oxygen for fibroblast function and bacterial defense. Poor circulation from cardiovascular disease, smoking, or vasculitis significantly extends healing. Smoking reduces wound oxygen tension by 25-30%, directly impairing healing processes. Smokers should understand that quitting even during recovery dramatically improves outcomes. Positioning and movement also influence circulation; construction workers should avoid prolonged immobility that compromises blood flow to injured areas.
Professional Assessment and Diagnosis
Accurate tunneling wound diagnosis requires skilled assessment beyond simple visual inspection. Healthcare providers use standardized techniques to determine tunnel extent, guide treatment planning, and monitor healing progress.
Physical Examination Techniques
During initial assessment, healthcare providers gently probe the wound opening using sterile instruments to determine tunnel direction, depth, and extent. This procedure, called “tunneling assessment,” must be performed carefully to avoid tissue damage or spreading infection deeper into tissues. Providers document tunnel characteristics using standardized terminology: location (measured by clock position if circular), depth (measured in centimeters), and direction (horizontal, vertical, or angled). Photography creates baseline documentation for comparing healing progress across weeks.
Imaging When Indicated
Simple tunneling wounds visible to physical examination typically don’t require imaging. However, complex injuries, suspected foreign body retention, or unclear wound anatomy may warrant ultrasound or MRI imaging. The American College of Radiology provides guidelines on imaging selection for wound evaluation. These imaging studies help identify retained debris, abscess formation, or tissue planes requiring surgical intervention.
Microbial Culture When Appropriate
If infection is suspected, wound culture identifies causative organisms and guides antibiotic selection. However, routine cultures of non-infected tunneling wounds aren’t necessary and may waste resources. Cultures become important when infection develops during healing, fever emerges, or wound appearance deteriorates despite appropriate care.
Treatment Protocols and Best Practices
Evidence-based treatment of tunneling wounds focuses on creating an optimal healing environment while preventing infection and complications.
Initial Wound Management
Immediate care following injury significantly impacts healing trajectory. First aid should include thorough irrigation with clean water or saline to remove contaminants. For construction injuries, this means flushing away dirt, rust, or other debris that could introduce infection. Avoid applying pressure that forces contaminants deeper into the tunnel. Once bleeding is controlled, professional evaluation should occur within 24 hours for proper cleaning and assessment. Tetanus status should be verified; construction workers should maintain current tetanus protection as part of occupational safety protocols.
Debridement and Surgical Intervention
Dead or devitalized tissue must be removed to promote healing and prevent infection. For tunneling wounds, this may require surgical exploration to visualize the entire tunnel, remove foreign material, and assess tissue viability. Sharp debridement using scalpels or curettes removes non-viable tissue efficiently. The Wound Healing Society recommends debridement within 48 hours of injury for optimal outcomes. In some cases, particularly complex tunneling wounds, surgical closure of the tunnel opening may be necessary after thorough cleaning.
Dressing Selection and Management
Appropriate dressing selection maintains optimal moisture, prevents infection, and facilitates monitoring. For tunneling wounds, several dressing categories serve different purposes:
- Gauze packing: Provides absorbency and allows visualization during frequent dressing changes; requires daily changes and careful packing to avoid pressure necrosis
- Foam dressings: Absorb moderate drainage while maintaining moisture; typically changed 2-3 times weekly
- Alginate or hydrofiber: Absorb copious drainage and conform to irregular wound shapes; excellent for deep tunneling wounds
- Negative pressure wound therapy: Applies controlled suction to promote healing in complex or slow-healing tunneling wounds; typically reserved for wounds not responding to standard treatment
Dressing changes should follow a consistent schedule determined by drainage volume and wound assessment. More frequent changes (daily) are appropriate for infected wounds or those with heavy drainage. As healing progresses and drainage decreases, change frequency can reduce to 2-3 times weekly.
Infection Prevention and Management
Maintaining sterile technique during dressing changes prevents introducing new pathogens. Healthcare providers should use clean or sterile gloves depending on wound classification. Hand hygiene before and after dressing changes is essential. If infection develops, systemic antibiotics become necessary alongside local wound care. Broad-spectrum antibiotics often start empirically while culture results pending; therapy can then narrow to targeted coverage once organisms are identified.
Prevention Strategies for Job Sites
Construction professionals can significantly reduce tunneling wound incidence through proper safety protocols and equipment maintenance.
Hazard Identification and Control
Sharp objects, machinery with pinch points, and contaminated surfaces create tunneling wound risk. Comprehensive OSHA hazard assessments identify specific risks on each job site. Engineering controls—such as machine guarding, tool storage systems, and work surface management—represent the most effective prevention method. Administrative controls including proper work procedures and supervision provide additional protection. Personal protective equipment (PPE) including puncture-resistant gloves and steel-toed boots provides the final layer of defense.
Proper Footwear and Hand Protection
Construction workers should wear appropriate PPE matching job-site hazards. Puncture-resistant soles protect against nail injuries, the most common cause of occupational tunneling wounds. Cut-resistant gloves with appropriate grip prevent hand injuries from sharp tools and machinery. However, PPE must be maintained properly; damaged gloves or worn soles lose protective value and require replacement.
Immediate Injury Response Protocols
When injuries occur despite prevention efforts, rapid response minimizes complications. Job sites should maintain well-stocked first aid kits with saline for irrigation, sterile gauze, and antibiotic ointment. Workers should receive training on basic wound care and know when to seek professional evaluation. Puncture wounds, regardless of apparent severity, warrant professional assessment within 24 hours. Establishing relationships with nearby urgent care facilities or occupational health clinics ensures workers can access prompt evaluation.
Return-to-Work Considerations
After tunneling wound treatment, workers should follow modified duty restrictions during healing. Continuing work in contaminated environments or with activities that compromise the wound risks infection and delayed healing. Most workers can return to modified duty within 1-2 weeks but shouldn’t return to full activity until wound closure is complete and scar tissue has matured (typically 4-6 weeks minimum). Gradual activity progression reduces reinjury risk.
Complications and Warning Signs
Understanding potential complications enables early intervention before serious problems develop.
Infection and Sepsis
Infection represents the most common tunneling wound complication. Signs include increasing pain, purulent drainage, foul odor, erythema, warmth, and systemic symptoms including fever and malaise. Untreated infections can progress to cellulitis, abscess formation, or life-threatening sepsis. Construction workers should seek immediate evaluation if infection signs develop. Early antibiotic therapy and aggressive wound drainage prevent progression to serious complications.
Chronic Wounds and Delayed Healing
Some tunneling wounds fail to progress through normal healing phases, becoming chronic wounds requiring prolonged treatment. Risk factors include poor nutrition, immunosuppression, inadequate wound care, or continued trauma to the area. Chronic tunneling wounds may require specialized interventions including negative pressure therapy, growth factor applications, or surgical reconstruction. When wounds aren’t noticeably improving after 2-3 weeks, specialist referral becomes appropriate.
Scar Formation and Contracture
All tunneling wounds heal with scarring; the question is whether scars form functionally or cause problems. Excessive collagen deposition can create hypertrophic scars or keloids, particularly in predisposed individuals or those with darker skin tones. Contracture—where scar tissue shrinks and limits movement—can occur if tunneling wounds involve joints or areas requiring significant mobility. Serial scar assessment guides whether interventions including silicone products, pressure garments, or surgical revision become necessary.
Hidden Abscess Formation
Occasionally, despite appropriate treatment, loculated infections develop within tunnel walls, forming abscesses that resist antibiotic penetration. These present as persistent pain, drainage, or fever despite treatment. Imaging and possible drainage procedures become necessary to resolve abscesses. This complication emphasizes the importance of initial thorough debridement and ongoing clinical assessment.
When considering how to approach DIY projects around your home, understanding proper wound care is essential for minor injuries. However, for significant tunneling wounds from construction accidents, professional medical evaluation remains non-negotiable. Just as basement finishing requires proper structural assessment before proceeding, wound management requires professional evaluation before self-care.
Construction workers managing job site injuries should recognize that tunneling wounds differ fundamentally from surface cuts. The hidden nature of tissue damage and infection risk demand professional assessment and monitoring. While home security requires consistent attention, wound security requires consistent professional oversight until complete healing confirms tissue integrity.
Understanding tunneling wound healing timelines and proper management represents essential knowledge for construction professionals. The 2-6 week standard healing timeline provides a baseline, but individual variation based on age, health status, infection, and injury characteristics means each wound requires personalized assessment. By recognizing warning signs, following evidence-based treatment protocols, and implementing prevention strategies, construction workers can minimize tunneling wound complications and achieve optimal healing outcomes.
FAQ
How long does a tunneling wound typically take to heal?
Most uncomplicated tunneling wounds heal within 2 to 6 weeks, though complex or infected wounds may require 8-12 weeks or longer. Healing duration depends on wound depth, contamination level, individual health status, and adherence to treatment protocols. Professional assessment provides personalized timeline estimates based on specific wound characteristics.
Can tunneling wounds heal on their own without professional treatment?
While minor tunneling wounds may eventually heal independently, professional evaluation and treatment significantly improve outcomes and reduce complications. The hidden nature of tunneling wounds makes infection risk substantial without proper assessment and management. Seeking professional care within 24 hours of injury prevents most serious complications.
What’s the difference between tunneling wounds and regular puncture wounds?
Puncture wounds create narrow channels with minimal surrounding tissue damage, while tunneling wounds develop extensive undermined areas beneath intact skin. This anatomical difference means tunneling wounds hide deeper infection risk and require more aggressive initial management including exploration and debridement.
How often should tunneling wound dressings be changed?
Dressing change frequency depends on drainage volume and wound characteristics. Early-stage tunneling wounds often require daily changes, while wounds with moderate drainage typically change 2-3 times weekly. As healing progresses and drainage decreases, change frequency reduces further. Healthcare providers recommend specific schedules based on individual wound assessment.
When should I see a specialist for a tunneling wound?
Initial evaluation should occur with a primary care provider or urgent care physician within 24 hours of injury. Specialist referral to wound care specialists, surgeons, or infectious disease physicians becomes appropriate if wounds don’t progress as expected, infection develops, or complications emerge. Wounds showing no improvement after 2-3 weeks warrant specialist evaluation.
Can construction workers return to work with a healing tunneling wound?
Workers can typically return to modified duty within 1-2 weeks if wounds are clean and healing appropriately. However, returning to full construction duties with contamination exposure or activities stressing the wound increases infection and reinjury risk. Most workers require 4-6 weeks minimum before resuming full job-site duties. Gradual activity progression prevents complications.
What nutritional support helps tunneling wound healing?
Protein (1.2-1.5g per kilogram body weight), vitamin C (500-1000mg daily), zinc (15-30mg daily), and adequate hydration all support healing. Construction workers should maintain balanced nutrition during recovery, with particular attention to these key nutrients. Nutritional supplementation may benefit workers with poor dietary intake or conditions affecting nutrient absorption.


