Dry Socket Healing Time: Dentist Insights and Recovery Guidelines
Dry socket, medically known as alveolar osteitis, is a painful complication that can occur after tooth extraction. When a blood clot fails to form or dislodges from the extraction site, the underlying bone and nerve become exposed to air, bacteria, and food particles. This condition affects approximately 2-5% of patients undergoing tooth extractions, though the rate increases to 10-40% for wisdom tooth removals. Understanding the healing timeline and proper care protocols is essential for anyone recovering from a dental extraction.
The healing trajectory for dry socket varies depending on the severity of the condition, individual healing capacity, and adherence to post-extraction care instructions. Most patients experience significant improvement within 7-10 days of treatment, though complete resolution may take 2-3 weeks. This comprehensive guide explores the healing timeline, contributing factors, and evidence-based management strategies recommended by dental professionals.
Understanding Dry Socket Development
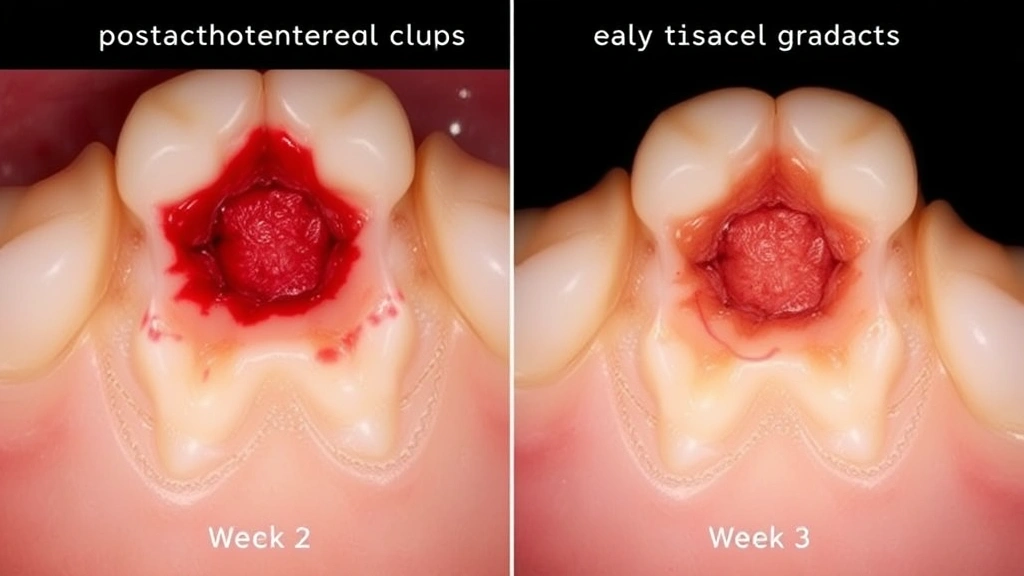
Dry socket occurs when the protective blood clot that normally forms in the extraction socket becomes compromised. This clot serves critical functions: it stops bleeding, protects the underlying bone and nerve tissue, and provides the foundation for new bone formation. When this clot fails to develop properly or becomes dislodged, exposed bone becomes susceptible to infection and inflammation.
The condition typically manifests 2-4 days after extraction, though symptoms can appear within 24 hours or as late as a week post-procedure. Patients typically report severe throbbing pain that radiates from the extraction site to surrounding areas of the jaw, ear, or temple. Unlike normal post-extraction discomfort that responds to over-the-counter pain medication, dry socket pain often requires prescription-strength treatment and professional intervention.
Risk factors include smoking, oral contraceptive use, poor oral hygiene, difficult extractions requiring bone removal, and previous history of dry socket. Understanding these risk factors helps patients and dentists implement appropriate preventive measures before complications develop. When considering your home improvement projects like DIY basement finishing, recovery time from dental procedures should factor into your planning timeline.
Typical Healing Timeline
Days 1-3: Initial Post-Extraction Phase
Immediately following tooth extraction, a blood clot forms within the socket. During this critical period, the extraction site should be protected from disturbance. Normal swelling, bruising, and mild discomfort are expected. If dry socket develops, symptoms typically emerge by day 2 or 3, manifesting as increasing pain rather than improving comfort. This is the critical window for distinguishing normal healing from complications.
Days 4-7: Peak Symptom Phase
If dry socket is present, this period usually features maximum pain intensity. The exposed bone becomes increasingly inflamed and vulnerable to secondary infection. Professional treatment during this phase is most effective, as early intervention prevents progression to more severe complications. With proper treatment initiated at this stage, patients typically experience pain reduction within 24-48 hours.
Days 8-14: Active Healing Phase
Following professional treatment, the extraction site begins active healing. New granulation tissue forms over the exposed bone, providing protection and initiating the healing cascade. Pain typically decreases substantially during this week, though complete resolution may not occur. Patients can gradually resume normal activities, though certain restrictions remain important for optimal healing.
Weeks 3-8: Bone Remodeling Phase
Complete healing involves complex bone remodeling processes that continue for several weeks. While symptoms resolve and the site appears healed externally, internal bone formation continues. Full bone healing typically requires 3-6 months, similar to the timeline for concrete curing timeframes in construction projects. However, functional recovery and return to normal activities occurs much earlier.
Factors Affecting Recovery Duration
Individual Healing Capacity
Patients with robust immune systems and good overall health typically experience faster resolution. Age, nutritional status, and underlying medical conditions significantly influence healing speed. Younger patients often heal more quickly, while those with diabetes, compromised immune function, or nutritional deficiencies may experience prolonged recovery.
Extraction Complexity
Simple extractions of single-rooted teeth have lower dry socket incidence and faster recovery compared to complex wisdom tooth removals requiring bone removal. The extent of surgical trauma directly correlates with inflammation duration and healing timeline. Impacted teeth requiring surgical extraction carry substantially higher complication risks.
Smoking and Tobacco Use
Smoking remains the most significant modifiable risk factor for dry socket development and delayed healing. Tobacco smoke impairs blood flow, increases infection risk, and compromises the blood clot’s integrity. Patients who continue smoking during recovery experience 4-12 times higher dry socket rates and slower overall healing. Cessation before extraction dramatically improves outcomes.
Oral Hygiene Practices
Meticulous post-extraction oral hygiene accelerates healing and prevents secondary infection. Gentle saltwater rinses beginning 24 hours post-extraction promote cleansing without disturbing the healing site. However, aggressive rinsing or touching the extraction area delays healing and increases complication risk.
Medication Interactions
Oral contraceptives increase dry socket risk by approximately 4-fold, likely through effects on fibrinolysis and clot stability. Patients using hormonal contraception should inform their dentist before extraction. Certain antibiotics and anti-inflammatory medications may also influence healing trajectories, making medication review essential for recovery optimization.
Professional Treatment Options
Professional treatment is essential for resolving dry socket and accelerating healing. Unlike normal post-extraction discomfort manageable at home, dry socket requires dental intervention for optimal outcomes.
Diagnosis and Assessment
Dentists diagnose dry socket through clinical examination, identifying exposed bone and characteristic symptoms. Radiographic imaging may rule out other complications like retained root fragments or infection. Proper diagnosis ensures appropriate treatment selection and prevents unnecessary interventions.
Alveolar Osteitis Treatment Protocols
The standard treatment involves gentle socket irrigation with saline solution to remove debris and bacteria, followed by placement of medicated dressings. American Dental Association guidelines recommend iodoform-based dressings combined with eugenol or other analgesic agents. These dressings require replacement every 2-3 days until healing progresses adequately.
Pain Management
Prescription-strength analgesics provide necessary pain control during active treatment. NSAIDs reduce inflammation while opioid medications address severe pain when necessary. Topical anesthetics applied to the extraction site provide temporary relief between professional treatments. Multimodal pain management combining medications, professional treatment, and home care provides optimal comfort during recovery.
Antibiotic Consideration
Antibiotics are prescribed when secondary infection is present or highly likely. However, prophylactic antibiotics without infection evidence are not routinely recommended, as they may promote antibiotic resistance without clinical benefit. Culture and sensitivity testing guides antibiotic selection when infection is confirmed.
For patients managing multiple health concerns simultaneously, understanding recovery timelines helps coordinate care. Just as planning home security improvements requires understanding project phases, dental recovery requires knowledge of healing stages.
Home Care and Management
Immediate Post-Extraction Care (First 24 Hours)
Bite pressure on gauze for 30-45 minutes helps establish initial clot formation. Avoid touching the extraction site, smoking, using straws, or engaging in strenuous activity. Apply ice packs for 15 minutes on, 15 minutes off during the first 24 hours to minimize swelling and inflammation.
Dietary Modifications
Soft, cool foods support healing while avoiding extraction site irritation. Avoid hot foods and beverages that increase blood flow and promote bleeding. Nutritious foods rich in vitamin C, zinc, and protein support immune function and tissue repair. Adequate hydration facilitates healing and helps prevent complications.
Oral Hygiene Protocol
Beginning 24 hours after extraction, gentle saltwater rinses after meals promote cleansing. Use 1/2 teaspoon salt dissolved in 8 ounces warm water, rinsing gently without vigorous swishing. Avoid the extraction site when brushing adjacent teeth. This careful approach maintains hygiene while protecting the healing clot.
Activity Restrictions
Strenuous exercise and heavy lifting increase blood pressure and promote clot dislodgement. Rest for 3-5 days allows initial healing before resuming normal activities. Gradually increase activity levels based on comfort and healing progression. Avoid sleeping flat; elevate your head with extra pillows to reduce swelling.
Medication Management
Take prescribed medications exactly as directed. Over-the-counter pain relievers help manage discomfort, though prescription medications may be necessary for dry socket. Anti-inflammatory medications reduce swelling and associated pain. Never exceed recommended dosages, and report concerning side effects to your dentist or physician.
Prevention Strategies
Pre-Extraction Optimization
Excellent oral hygiene before extraction reduces bacteria and infection risk. Address any active infections before extraction when possible. Discuss all medications and supplements with your dentist, as some affect clotting. Optimize nutritional status and overall health before elective extractions.
Smoking Cessation
Cessation at least 1-2 weeks before extraction dramatically improves outcomes. Ideally, quit smoking permanently to improve overall health and prevent future complications. Even temporary cessation during the critical healing window substantially reduces dry socket risk. Your dentist can provide cessation resources and support.
Surgical Technique Optimization
Experienced dentists use gentle techniques minimizing trauma and preserving blood supply. Careful socket management, avoiding excessive bone removal, and precise closure techniques reduce dry socket incidence. Complex cases may warrant referral to oral surgeons with specialized training.
Post-Operative Instructions Adherence
Following all post-extraction instructions precisely prevents complications. This includes activity restrictions, dietary modifications, medication timing, and follow-up appointment attendance. Clear communication with your dental team ensures you understand all recommendations and can implement them effectively.
Professional Follow-Up Care
Scheduled follow-up appointments allow dentists to monitor healing and identify complications early. These visits provide opportunities to replace medicated dressings, assess pain management adequacy, and adjust care protocols as needed. Regular monitoring significantly improves outcomes and accelerates healing.
Understanding healing timelines helps coordinate dental care with other commitments. Similar to planning DIY house painting projects with proper preparation phases, dental recovery requires planning and adherence to care protocols.
FAQ
How long does dry socket typically take to heal with professional treatment?
With professional treatment initiated promptly, most patients experience significant pain reduction within 24-48 hours. Complete healing typically requires 7-10 days of active treatment, with full resolution in 2-3 weeks. However, individual timelines vary based on healing capacity and treatment adherence.
Can dry socket heal on its own without professional treatment?
While some cases may eventually resolve independently, professional treatment dramatically accelerates healing and reduces suffering. Untreated dry socket risks secondary infection, prolonged severe pain, and potential bone complications. Professional intervention is strongly recommended for optimal outcomes.
What pain level is normal after tooth extraction versus dry socket?
Normal post-extraction discomfort gradually improves daily and responds to over-the-counter pain medication. Dry socket pain typically worsens after initial improvement and requires prescription-strength medication. Pain radiating to ear or temple, fever, or foul odor indicate complications requiring immediate professional evaluation.
Can dry socket recur after treatment?
Recurrence is uncommon when proper treatment is completed and post-care instructions are followed. However, patients with previous dry socket have slightly elevated risk for future occurrences. Preventive measures are particularly important for these patients.
Should I take antibiotics for dry socket?
Antibiotics are prescribed only when infection is present or highly likely, based on clinical assessment. Prophylactic antibiotics without infection evidence are not routinely recommended. Your dentist will determine appropriate antibiotic therapy based on examination findings and clinical judgment.
What foods should I avoid during dry socket healing?
Avoid hard, crunchy, hot, or spicy foods that irritate the extraction site or increase blood flow. Exclude foods requiring chewing near the affected area. Stick to soft, cool, nutrient-dense options like yogurt, smoothies, mashed vegetables, and protein-rich broths. Avoid alcohol and carbonated beverages.
How does smoking affect dry socket healing time?
Smoking dramatically increases dry socket risk and prolongs healing when complications develop. Tobacco smoke impairs blood flow, compromises immune function, and destabilizes blood clots. Patients who continue smoking experience significantly longer recovery compared to non-smokers.
When should I contact my dentist about post-extraction concerns?
Contact your dentist immediately if you experience severe pain unresponsive to medication, fever, foul odor from the extraction site, excessive bleeding beyond 24 hours, or signs of infection. These symptoms require prompt professional evaluation and treatment to prevent serious complications.


